What is an Adrenal Incidentaloma?
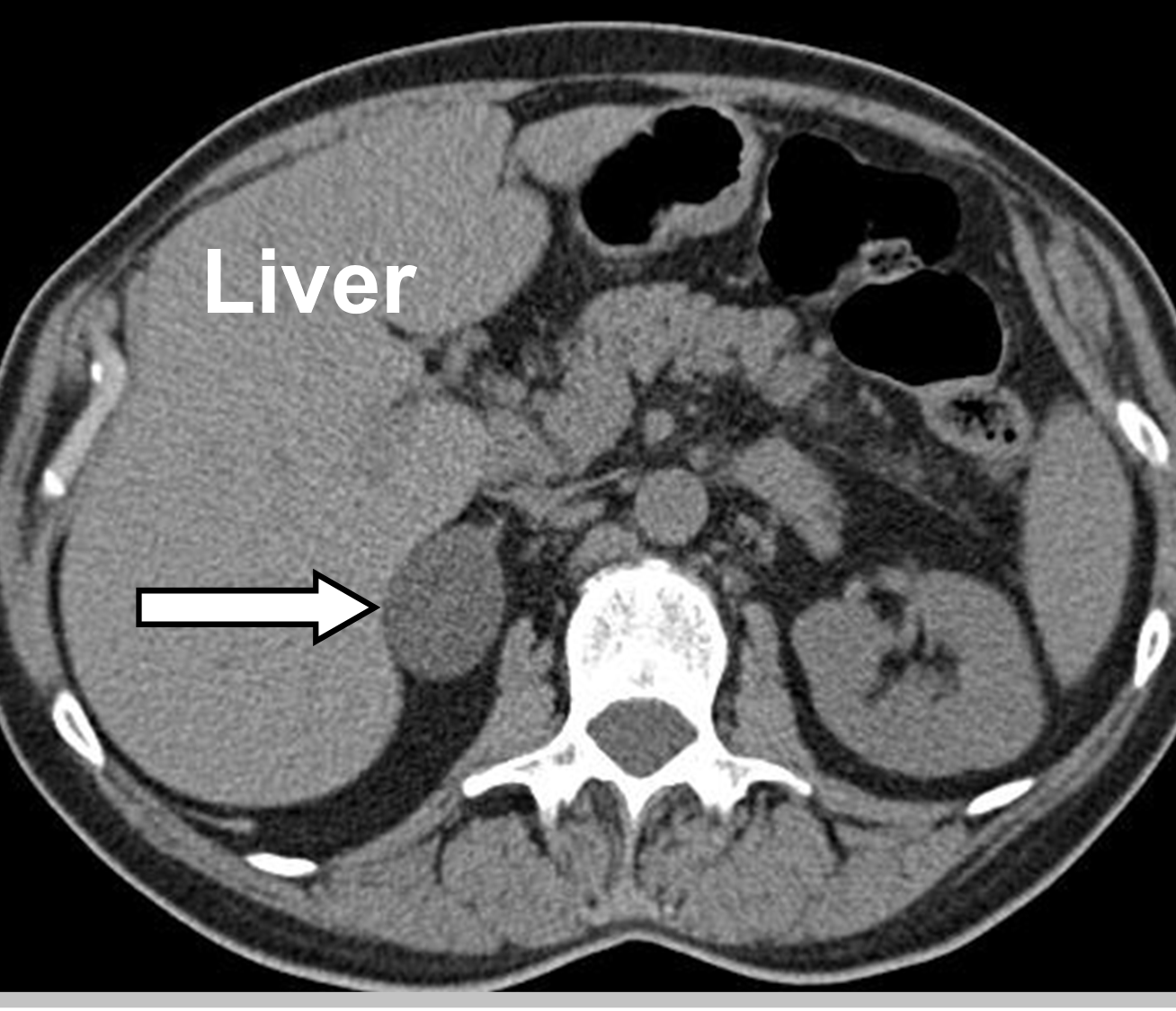 CT scan showing a right adrenal incidentaloma. All incidentally identified adrenal tumors seen on CT scans done in the ER need to be worked up to ensure they do not overproduce hormones or are cancerous.
CT scan showing a right adrenal incidentaloma. All incidentally identified adrenal tumors seen on CT scans done in the ER need to be worked up to ensure they do not overproduce hormones or are cancerous.
Is this bad?
Most of the time it is not bad at all and can be ignored. But further testing is usually necessary to make sure. It is important to know that about 90% of adrenal masses seen on a CT scan are benign growths that are not cancerous, do not make excess adrenal hormones, and thus they do not need to be removed. Most of the time they can be ignored moving forward. However, the primary thing for you to know is that a few blood and urine tests are typically necessary to determine if your adrenal mass is one of the 10% that should be removed, or is one of the 90% that do not need to be treated. The blood and urine tests will determine what needs to be done.
The HCA Care Assure Adrenal Tumor Screening Program
HCA Hospitals on the west coast of Florida want to make sure that patients who had an adrenal growth or adrenal tumor noted on a CT scan when visiting an HCA Hospital ER is followed up appropriately. This page will discuss this program and what it means to you, what you need to do, what doctors you need to see, and what tests you can be expected to undergo. The goal is to make sure all adrenal masses and growths are identified and tested appropriately to help you have the best care possible. The program HCA Hospitals created to achieve these goals is called Care Assure.
 HCA Hospitals are screening for adrenal tumors through their Care Assure program.
HCA Hospitals are screening for adrenal tumors through their Care Assure program.
How does the HCA Care Assure Program for adrenal tumors work?
HCA Hospitals began their Care Assure program to make sure patients get the best treatment possible for issues identified during a visit to one of their hospitals. This program was needed because many times the patient went to the hospital and got a CT scan for some other reason, and the adrenal mass was seen incidentally. In other words, they were not looking for an adrenal mass, but they found one. World wide, when something is found that wasn't the reason the patient came to the hospital then the "new" "incidental" problem often doesn't get the attention it deserves once the patient leaves the ER.The Care Assure program was designed to help patients who have an adrenal mass found on a CT scan receive the care they need, improving the efficiency of medical care and improving the overall quality of care and patient satisfaction. After an adrenal mass is found on a CT scan, a nurse navigator will contact you from the HCA hospital and tell you what the correct next steps are. In addition, the nurse navigator will communicate with both your hospital doctors and your regular doctors (including the primary care physician) to help you navigate and schedule appointments, laboratory studies and any other tests you may need.
Why is it important that adrenal masses found on CT scan are investigated?
Even though the overwhelming majority of adrenal tumors are benign, many of them cause significant and often dramatic symptoms because they produce excess adrenal hormones. Adrenal tumors that produce hormones always need to be removed because the excess hormones can cause toxic effects to your body, make you feel miserable and cause early death. Too much adrenal hormones such as aldosterone, cortisol and catecholamines (adrenaline-type hormones) can create very toxic effects on the body long-term.Adrenal tumors that make too much hormone are called “functioning” or “endocrine-active” tumors. Aldosterone producing adrenocortical tumors cause primary hyperaldosteronism (also called Conn's Syndrome, whereas cortisol producing adrenocortical tumors cause primary hypercortisolism or Cushing's Syndrome. Catecholamine (epinephrine and adrenaline) producing adrenal tumors cause pheochromocytoma. Any functioning adrenal tumor should be removed by surgery (adrenalectomy). Cancerous and potentially cancerous masses are also removed with surgery. The vast majority of adrenal tumors are benign, meaning not cancerous, but still may need to be removed if they are making too much of any adrenal hormone. You can read more about all of these adrenal tumors by selecting them in our navigation menu.
Questions to Ask Your Doctor
- What tests do I need?
- Is my adrenal tumor producing excess hormone?
- Should I see an endocrinologist?
- What are my options for treatment?
- If surgery is required, is there an expert in adrenal surgery?
- How often will I need check-ups?
What are some of the test I may need for an adrenal mass?
First, in addition to the CT scan you already had, it is important for you to meet with your doctor to assess via a History and Physical Examination (H&P) whether you have any adrenal-specific signs and symptoms of adrenal disease. A great doctor will always perform a very careful H&P to identify signs and symptoms of adrenal tumor disease. One of the hallmarks of adrenal tumors is high blood pressure, also known as hypertension. Most adrenal tumors that are producing hormone will cause high blood pressure. Tumors that overproduce catecholamines (called pheochromocytoma), as well as aldosterone-producing tumors (aldosteronoma or Conn's tumor) and cortisol-producing tumors (causing Cushing's syndrome) can all cause high blood pressure.Many patients with a pheochromocytoma have a variety of symptoms. They can have spells that are extremely variable with differing symptoms each time, but the symptoms typically include heart palpitations, pallor, flushing, tremors, headaches and sweating. They get sweaty, their heart races and they have anxiety. If the adrenal tumor is overproducing cortisol, you will develop symptoms of Cushing’s syndrome. The symptoms of Cushing’s syndrome include weight gain and central body obesity (you store fat especially around your abdomen). Your face might develop more round features and you develop fat deposits above your collar bones and on your back (called buffalo hump). Patients may develop problems with bruising easily, thin skin and poor wound healing. To read more about adrenal symptoms Click Here.
Second, there are a number of blood and urine test that neeed to be measured, each tailored to identify overproduction of any of the hormones, catecholamines (adrenaline), aldosterone and cortisol. To read more about adrenal lab testing Click Here. At a minimum you need to have the following laboratory tests:
Third, sometimes additional imaging is needed to better address the adrenal mass. However, this is very rare. In almost all cases a CT scan demonstrating the adrenal tumor is all you need. To read more about adrenal imaging Click Here.
Should I see a medical endocrinologist for the adrenal mass?
Medical endocrinologists are specialized medical doctors focusing on hormone-related diseases including adrenal tumor disease. The nurse navigator will communicate directly with your primary care physician. If needed, the nurse navigator can also assist in identifying and provide referrals to a medical endocrinologist. The medical endocrinologist can assist in ordering and interpreting the CT scan well as the adrenal tumor disease-specific blood and urine test.
What happens if I may need surgery for the adrenal mass?
The majority of adrenal tumors that are found incidentally on CT scan performed at a hospital ER will not need surgery. All will need to have their hormone production measured, and if none is being made, then all under 3cm will be able to be watched. All you may need to do is get another CT scan in 6 months or a year to make sure it is not growing. If the adrenal tumor is over 3 cm, or is producing any of the above hormones then surgery will almost always be recommended.If you need surgery, your doctors (usually the primary care physician and/or medical endocrinologist) will refer you for surgery. To read more about adrenal surgery Click Here. As you will read, it is extremely important for you to have a surgeon that performs adrenal surgery regularly, and unfortunately there are very few surgeons who do this.